

One of the reasons that so many children are being hospitalized and an
unacceptable number are dying from
asthma is that unfortunately there is
no advanced technology to help alert children and their caretakers of a
possible asthma attack. Regular monitoring of an asthmatic child’s lung
function is extremely important, and the monitoring method most
prescribed involves the use of peak fl ow
meters. Peak flow meters are hand–held devices that can measure a
child’s ability to push air out of their lungs when they blow forcefully
into the meter. Although measurements from peak flow meters can signal
a looming asthma attack, the problem is that children under six
are too young to properly use peak flow meters, and many children
over six find them a nuisance to carry around and therefore do not
use them routinely.
ow
meters. Peak flow meters are hand–held devices that can measure a
child’s ability to push air out of their lungs when they blow forcefully
into the meter. Although measurements from peak flow meters can signal
a looming asthma attack, the problem is that children under six
are too young to properly use peak flow meters, and many children
over six find them a nuisance to carry around and therefore do not
use them routinely.
Some medical professionals have recommended the use of pulse oximeters
that measure the percentage of hemoglobin in the blood saturated with
oxygen as another means of managing asthma. This technology is
impractical for several reaso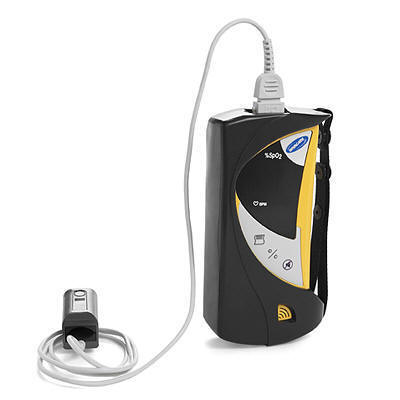 ns.
First of all, many oximeters are not portable. For
a pulse oximeter to work
properly, a probe from the pulse oximeter must be attached to a child’s
finger or ear lobe and then connected to a computerized unit. Two
different wavelengths of light then come from the probe and are absorbed
by the hemoglobin in the child’s blood. The amount of light absorbed by
the hemoglobin depends upon how saturated it is with oxygen. The
information is sent back to the computerized unit which computes the
percentage of hemoglobin saturated with oxygen. Secondly the pulse oximeter, costing around $1500, is impractical because it is too costly
for the average person.
ns.
First of all, many oximeters are not portable. For
a pulse oximeter to work
properly, a probe from the pulse oximeter must be attached to a child’s
finger or ear lobe and then connected to a computerized unit. Two
different wavelengths of light then come from the probe and are absorbed
by the hemoglobin in the child’s blood. The amount of light absorbed by
the hemoglobin depends upon how saturated it is with oxygen. The
information is sent back to the computerized unit which computes the
percentage of hemoglobin saturated with oxygen. Secondly the pulse oximeter, costing around $1500, is impractical because it is too costly
for the average person.
Home History
Future Technology
Design Process
Breakthroughs
Consequences Bibliography